Case Studies
These case studies highlight the clinical utility of the Autoimmune Brain Panel™ in patients with complex neuropsychiatric presentations. Each case demonstrates how test results helped identify underlying immune dysfunction and assisted in guiding targeted treatment ─ leading to symptom improvement or resolution.
One simple blood draw – ordered by your provider – may put you on the path to recovery.
Case Study #1:
Autoimmune-induced neuropsychiatric symptoms in an 8-year-old female
Antibiotic treatment leads to resolution of multiple neurologic and psychiatric symptoms
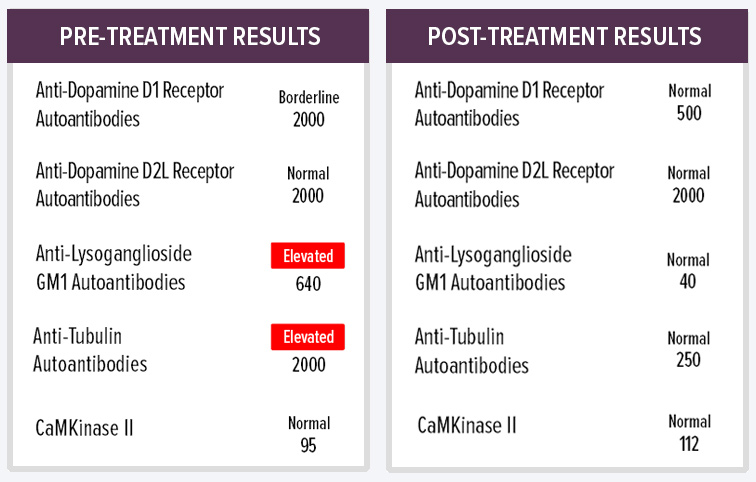
Presenting Symptoms: 8-year-old girl with abrupt onset of obsessive-compulsive behaviors, vocal tics, poor concentration, sensory/motor abnormalities, emotional lability, regression, aggression, and dysgraphia. Parents report urinary and sleep problems.
Course of Illness: Relapsing and remitting symptoms with improvement after 2-3 days of azithromycin.
Previous Diagnosis: Anxiety, OCD, unspecified disorder of immune mechanism
Medical History: Significant for two recent streptococcal infections with high fever, sore throat, sinus pain and cough. History of frequent ear infections, sinus infections and idiopathic fevers.
Treatment: Azithromycin with rapid symptom improvement.
Status: All symptoms resolved. Returned to baseline after 2-3 days of treatment.
Case Study #2:
Gradual onset of tics and severe cognitive regression in 20-year-old male
Initially diagnosed with bipolar disorder, testing reveals immune-mediated condition
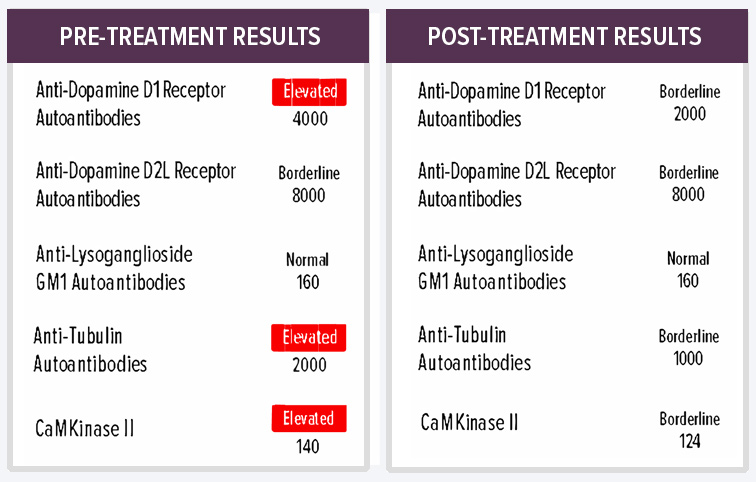
Presentation: 20-year-old male with gradual onset of tics, inability to concentrate, sensory abnormalities, emotional lability, severe cognitive regression, separation anxiety, developmental regression, sleep disturbances, handwriting disturbance and aggressiveness.
Previous Diagnoses: Unspecified bipolar disorders
Previous Lab Results: Positive for Lyme disease, Babesia, and Rickettsia
Medical History: Rocky Mountain Spotted Fever, multiple ear and strep infections throughout childhood, known immunodeficiency.
Treatment: Plasmapheresis followed by multiple IVIg treatments.
Status: Overall cognitive abilities improved, with mother reporting patient’s math skills returned after many years.
Case Study #3:
Severe OCD and tics improve with immune-modulatory treatment
Clinical and laboratory results support autoimmune-based illness
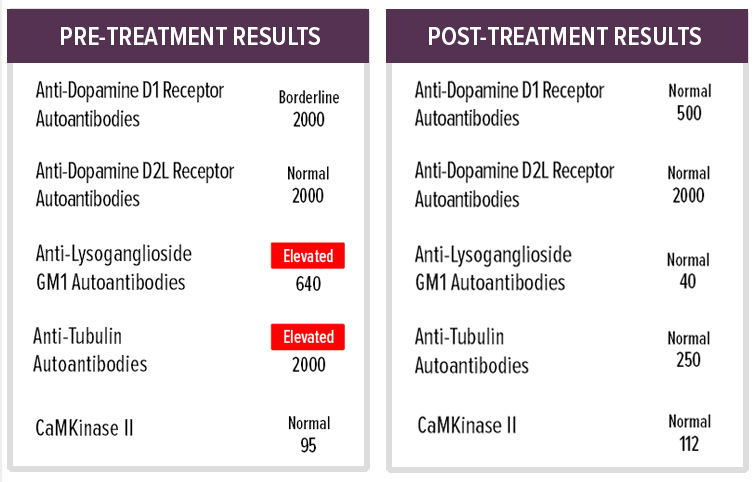
Presentation: 16-year-old female with abrupt onset at age 11 of severe OCD (food restriction), tics and choreiform movements, poor concentration, significant cognitive and academic decline, sensory abnormalities, severe mood dysregulation, urinary urgency and frequency, and dysgraphia. Aggressive behaviors prompted 6 calls to local police for assistance.
Course of Illness: Relapsing and remitting symptoms with three major episodes reported. Sudden increase in symptoms with strep exposure.
Previous Diagnoses: Autoimmune disease NOS, post-infectious encephalitis and encephalomyelitis, other diseases involving the immune system NOS
Previous Lab Results: Positive Lyme Western blot, elevated Mycoplasma and Coxsackie titers
Status: Symptom improvement