New-onset seizures associated with Lyme Disease
Published Study: Autoimmune Epilepsy Temporally Associated with Lyme Disease: A Report of Two Cases
Autoimmune epilepsy associated with Lyme disease is an emerging concept in which seizures may be driven by an underlying autoimmune dysfunction, triggered by infection. This article describes a 25-year-old male and 14-year-old female, who developed new-onset seizures temporally associated with Lyme-associated illness, which resolved after antimicrobial and immunomodulatory treatments.
Seizures don’t respond to treatment
In one case, the author describes a previously healthy 14-year-old female who developed new-onset myoclonic seizures following travel to the Caribbean, where she reported exposure to ticks and sand fleas. Her initial episodes were characterized by brief, shock-like jerks affecting both the upper and lower extremities. Serologic testing returned positive for Lyme disease, and EEG demonstrated generalized irregular spike-and-wave activity.
However, seizures persisted despite anti-seizure medications and worsened after starting antibiotic treatment for Lyme disease.
“Within approximately two weeks of antimicrobial initiation, seizure frequency increased from roughly one event per month to several events per week.” 1
Autoimmune Brain Panel™ helps detect underlying immune dysfunction
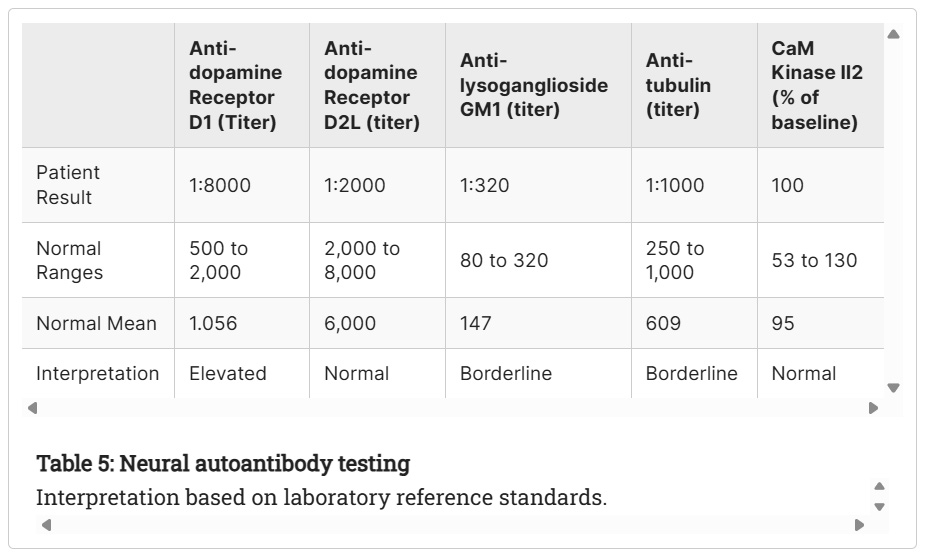
Given concern for an immune-mediated process, the Autoimmune Brain Panel™ (formerly the Cunningham Panel™) was ordered. The results demonstrated elevated anti-dopamine receptor D1 antibodies, with borderline anti-Lysoganglioside GM1 and anti-tubulin antibodies, findings that supported an underlying autoimmune dysfunction.
With persistent, treatment-refractory seizures and evidence of immune dysfunction, the patient was treated with intravenous methylprednisolone followed by IVIG, while continuing antimicrobial therapy.
“By six weeks, she was seizure-free. At six-month follow-up, she remained seizure-free without antiseizure medication and continued on doxycycline, 100 mg twice daily.” 1
“Although these findings do not establish a causal relationship between Lyme disease and autoimmune epilepsy, they suggest that infection-associated immune dysregulation may contribute to seizures in selected patients.” 1
References
- Source: Cipriano P M (March 14, 2026) Autoimmune Epilepsy Temporally Associated With Lyme Disease: A Report of Two Cases. Cureus 18(3): e105228. doi:10.7759/cureus.105228
Join Dr. Craig Shimasaki for a webinar on the biology of infection-triggered autoimmune neuropsychiatric disorders and the clinical use of the Autoimmune Brain Panel™ (formerly the Cunningham Panel™) for diagnosis and treatment.
Webinar: When Standard Treatments Fail: How Infections and Immune Dysfunction Trigger Neuropsychiatric Symptoms
When: Tuesday, June 16 at 6pm CT
Learn how the Autoimmune Brain Panel™ can help identify patients whose neuropsychiatric symptoms may stem from an infection-triggered autoimmune process.
Schedule your free, personalized 1-on-1 consultation with our Medical Relations Manager Amy Cross, NP.
RELATED STUDIES
(Bransfield R., et al. Healthcare. December 29, 2023)
A wide range of microbes—including bacteria, viruses, fungi, and parasites—have been associated with conditions such as autism spectrum disorder, schizophrenia, bipolar disorder, depression, anxiety, suicidality, and behavioral dysregulation, often through mechanisms involving neuroinflammation, immune activation, and altered gene expression.
(Breitschwerdt E., et al. Journal of Central Nervous System Disease. March 18, 2019)
An adolescent with severe, treatment-resistant psychosis for 18 months showed progressive improvement of neuropsychiatric symptoms, was able to discontinue psychiatric medications, and returned to pre-illness activities following combination antimicrobial therapy. He also experienced a resolution of Bartonella-associated skin lesions.
(Cross A., et al. Frontiers in Psychiatry. February 2, 2021)
A 7-year-old girl developed relapsing neuropsychiatric symptoms after travelling to a tick-endemic area. She tested positive for Lyme disease and multiple streptococcal infections, meeting PANDAS criteria. After 31 months of antimicrobial therapy and IVIg, she achieved complete remission and remained symptom-free at the time of publication.




